By Pooja Babbrah, Practice Lead, PBM Services
Specialty medications are changing health care, providing life-saving treatment options for patients with rare and chronic conditions. Patients, however, often face big hurdles in obtaining specialty medications, creating inefficiencies that delay start to therapy or force patients/doctors to abandon first-line therapies.
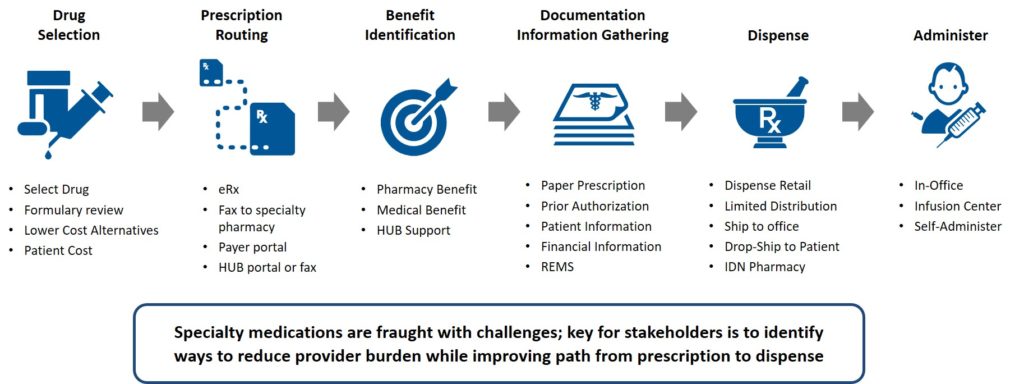
Standards Enhancements to Bring Specialty Pharmacy Into Digital World
The good news is that healthcare industry standards are being enhanced to bring specialty pharmacy into the digital world by both NCPDP and HL7. These improvements will dramatically reduce provider burden and the path from prescribe to dispense.
On the NCPDP front, the new Specialty Pharmacy Work Group (that I co-chair) is working to identify pain points and transactions that delay the prescribing, enrollment, dispensing, care management, reporting and payment of specialty medications. Three focus areas that have momentum are:
- Specialty Enrollment – This is primarily a paper form that specialty pharmacies use to capture the demographic, insurance, medication and clinical information needed to get therapies to patients. It can range from one to multiple pages of information, depending upon the pharmacy, manufacturer and condition. This task group is looking at using HL7 for extracting some of the clinical elements for the specialty enrollment transaction. Pharmacies and EHR vendors should have a voice at the table and/or be monitoring impacts to product development roadmaps.
- REMS – Risk Evaluation and Mitigation Strategies (REMS are mandated for certain specialty medications by the Food and Drug Administration (FDA). While REMS standards exist, translating REMS into action currently requires a lot of leg work and paperwork on the part of manufacturers, pharmacies, providers and patients. CMS has a renewed interest in getting stakeholders to implement existing NCPDP REMS transactions to lessen the burden on physicians and patients. NCPDP task groups are looking at how the REMS and specialty enrollment transaction can work together to streamline processes.
- Real-Time Pharmacy Benefit Check (RTPBC) – The RTPBC will provide transparent and up-to-date information on out-of-pocket costs and insurance coverage for the drugs covered under a patient’s pharmacy benefit. Interest in the RTPBC is accelerating because of adoption of a “Real-Time Benefit Tool” by Medicare Part D. This NCPDP transaction is expected to be balloted and approved this Fall.
In a future blog, we will look at specialty prescribing pain points that will be addressed by HL7 FHIR. In the meantime, if your organization needs help understanding the impact of emerging standards or use cases that will impact specialty pharmacy and your provider workflows or want to know more about NCPDP’s Specialty Pharmacy Workgroup, reach out to me, Pooja Babbrah, at pooja.babbrah@pocp.com.




